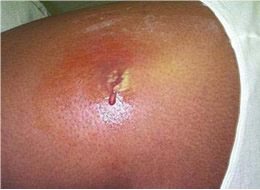
One of the keys to preventing the spread of the antibiotic-resistant skin infection or "super bug" known as
methicillin-resistant staphylococcus aureus ("MRSA") is proper identification and treatment of suspicious skin lesions. The infection often looks like an ordinary skin wound or boil, which may look harmless but rapidly develops into large abscesses within 24 to 48 hours.
Diagnosis is difficult
Treatment with penicillin-related antibiotics is ineffective. Coaches, parents, and athletes should therefore be on the lookout for:
- Skin
infections that may appear as pustules or boils at the site of visible
skin trauma, such as cuts and abrasions, and areas of the body covered
by hair (e.g. back of neck, groin, buttock, armpit, beard area);
- Fever;
- Pus or other drainage;
- Swelling; and/or Pain
MRSA: Suspicious Skin Infections
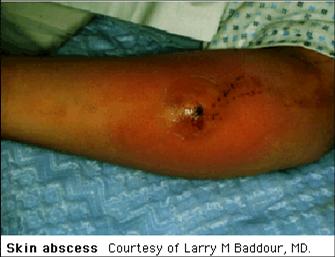
- localized collection of pus associated with tissue destruction
- can become super-infected
- body shaving, especially areas covered by clothing,
predisposes to infection
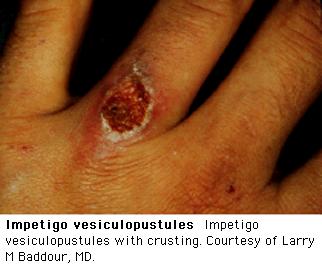
- Infection
of the skin surface without pus formation
Impetigo:
"It's important for coaches and
parents to be aware MRSA might be a cause of skin problems in
children," Dr. Dan Jernigan, a CDC medical epidemiologist, told the
Associated Press.
Treatment
If your child has a suspicious skin/soft tissue infection, take him to the doctor, who should obtain a culture of the lesion, which will guide selection of the appropriate antibiotic.
- The primary treatment of an abscess or purulent skin lesion (one discharging pus) is incision and drainage.
- Although this is usually adequate to clear up the infection, it is sometimes insufficient, in which case a course of antibiotics will be necessary.
- Antibiotic therapy may include clindamycin , trimethoprim-sulfamethoxazole (TMP-SMX, Septra, Bactrim) , and tetracycline .
- Using antibiotics following the incision and drainage of the lesion is left to the discretion of the treating physician based on the size of the lesion, cellulitis, age of the patient, fever, signs of systemic infection, and the presence and effect of other disorders or diseases.
Other prevention tips
- Clean and cover all wounds.
If an athlete's skin is injured, it should be washed immediately with
soap and warm water, dried and covered with a clean bandage. If a wound
cannot be covered adequately, the program should consider excluding
players with potentially infectious skin lesions from practice or
competition until the lesions are healed or can be covered adequately;
- Exclude infected athletes from participation. Athletes
with evidence of spreading, cellulitis or systemic infections (i.e.
fever and chills) should be excluded from sports participation.
Athletes with contained infections but no systemic symptoms may be able
to participate on a case-by-case basis.
- Anti-bacterial ointment. Clean
any cut with soap and water and then applying a topical
over-the-counter "maximum strength" or "triple antibiotic"
anti-bacterial ointment. While there are, as of yet, no
peer-reviewed clinical studies to confirm the results, a laboratory study conducted
at the College of Pharmacy at Oregon State University (OSU), which was presented
at a December 2007 meeting of the American Society of Health-System
Pharmacists, found that an ointment containing benzethonium chloride
with tea tree and white thyme oil worked best against all four tested
MRSA strains, while ointments containing neomycin, polymyxin, and
gramicidin also had some antibacterial effectiveness
Source: Centers for Disease Control; Weber, Kathleen. "Community-Associated Methicillin-Resistant Staphylococcus aureus Infections in the Athlete." Sports Health: A Multidisciplinary Approach 1 (2009): 405-410.
Teaser title:
MRSA: Spotting Infection Prevention, Treatment Key
Teaser text:
One of the keys to preventing the spread of the antibiotic-resistant skin infection or "super bug" known as methicillin-resistant staphylococcus aureus (MRSA) is proper identification and treatment of suspicious skin lesions. The infection often looks like an ordinary skin wound or boil, which may look harmless but rapidly develops into large abscesses within 24 to 48 hours. Diagnosis is difficult. Treatment with penicillin-related antibiotics is ineffective.